Bone Grafting In Pittsburgh

At Pinnacle Center Dental Implants and Periodontics, we provide exceptional bone grafting procedures designed to restore oral health and enhance the success of dental implants in Pittsburgh, PA. Our experienced periodontists, Dr. Katherine L. Roll and Dr. Kelly B. Williams, employ state-of-the-art technology and personalized care to deliver optimal results for every patient.
From the initial consultation
to post-procedure care,
we are here to support you
every step of the way.
Understanding Bone Grafting
Bone grafting is a sophisticated surgical procedure aimed at rebuilding or regenerating bone tissue that has deteriorated or diminished due to periodontal disease, tooth loss, trauma, or other dental conditions. It involves placing new bone material in areas lacking sufficient bone, prompting natural bone regeneration. As the bone heals, it creates a stable and robust foundation that is ideal for dental implants, ultimately leading to improved oral function, appearance, and health.
Our team is ready to help you achieve the smile you’ve always dreamed of.
Reasons Bone Grafting May Be Necessary
Bone grafting can be required for various reasons, including:
Dental Implant Preparation
Dental implants require a sufficient amount of healthy jawbone to anchor securely. Patients who have experienced bone loss due to prolonged tooth absence or advanced gum disease may need bone grafting to ensure the success and stability of dental implants.



There are various techniques to re-build bone tissue in order to ensure there is a solid foundation for a dental implant. Call us for a consultation today.
Advanced Gum Disease (Periodontitis)
Severe gum disease often leads to the deterioration of jawbone structure, causing teeth to become unstable. Bone grafting can restore bone strength, aiding in tooth preservation and overall oral health recovery.
Following Tooth Extractions
Tooth extraction can leave behind gaps and decrease bone density over time. Bone grafting immediately following extraction helps prevent bone loss, maintaining the jawbone’s integrity for future dental treatments, including implants.
Recovery from Oral Trauma or Injury
Injuries to the jaw or facial structure can result in significant bone loss. Bone grafting procedures help rebuild affected areas, restoring both function and appearance.
We are committed to delivering
Excellence in Dental Care


Trust our expert team to
help you achieve a smile
that reflects your true self
Excellence and Expertise


With dental implants, you can restore your smile, regain your confidence, and enjoy all the benefits of having strong, healthy teeth.
Types of Bone Grafts Offered
At Pinnacle Center, we offer several different types of bone grafts, each tailored to meet the unique needs of individual patients:
- Autogenous Bone Grafts – Also known as autografts, these involve using the patient’s own bone harvested typically from another area within the mouth. This approach ensures maximum compatibility and effectiveness.
- Allografts – Allografts involve sterilized, safe donor bone material, extensively screened to ensure patient safety. This approach eliminates the need for harvesting bone from your own body, minimizing surgical sites.
- Xenografts – These grafts use bone materials derived from animals, which are meticulously processed and sterilized. Xenografts integrate effectively with human bone, stimulating natural bone growth.
- Alloplastic Grafts – A synthetic, biocompatible option made from materials like calcium phosphate. Alloplastic grafts offer consistent quality, reliability, and strong support for new bone growth.
Bone Grafting Procedure
Our bone grafting process is thorough and patient-centered, comprising several key steps to ensure safety, comfort, and successful outcomes:

Comprehensive Consultation & Examination
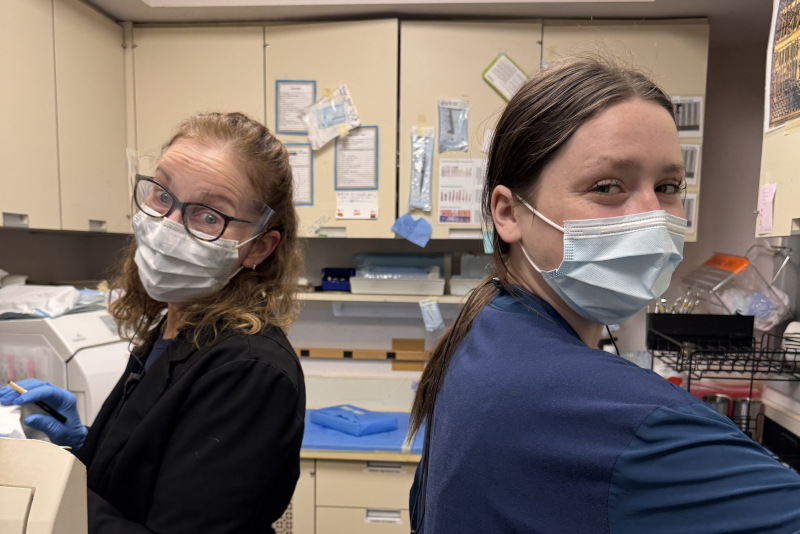
Dr. Roll or Dr. Williams will conduct a detailed consultation, including a thorough examination and advanced imaging techniques such as 3D Cone Beam CT scans. This assessment determines the health of your jawbone and the extent of bone loss.

Customized Treatment Planning
Based on your unique needs and imaging results, our periodontists will create a customized treatment plan, carefully selecting the type of bone graft most appropriate for your situation.

Performing the Bone Grafting Procedure
The bone graft material is carefully positioned into the targeted area during a gentle surgical procedure. Our doctors prioritize patient comfort, utilizing sedation options and local anesthesia as necessary.

Healing and Bone Integration
Following the procedure, your body naturally integrates the graft material, forming new, healthy bone. Healing duration varies based on the type of graft, individual health factors, and specific patient needs, typically ranging from several weeks to a few months.

Dental Implant Placement
Once the grafted area has healed and the new bone has solidified, the jawbone is ready for dental implant placement. This strengthened foundation supports dental implants securely, providing long-lasting, reliable tooth replacements.
Benefits of Bone Grafting
Patients undergoing bone grafting experience numerous benefits, including:
- Enhanced jawbone strength and density
- Significantly improved eligibility and success rate for dental implants
- Restoration of natural facial contours and aesthetics
- Improved oral functionality, such as chewing and speech
- Prevention of further deterioration of jawbone and oral health issues
- Increased confidence and self-esteem from a revitalized smile
Never again suffer from the use of dentures, or the pain and embarrassment of missing teeth. Ever!

Frequently Asked Questions
How long does bone grafting take to heal?
Healing typically takes anywhere from several weeks to a few months, depending on individual health factors and the type of graft used.
Is bone grafting painful?
Most patients experience minimal discomfort, effectively managed with sedation, local anesthesia, and prescribed pain medication following the procedure.
Can bone grafts fail?
Although rare, bone graft failure can occur due to infections, poor healing, or inadequate aftercare. Our periodontists ensure rigorous pre- and post-procedure care to minimize such risks.
Is everyone a candidate for bone grafting?
Most individuals with sufficient overall health are candidates. A comprehensive assessment will determine your eligibility.
How long does the procedure take?
The surgical procedure typically takes between one to two hours, depending on the complexity and the number of graft sites.

CHECK OUR
Patient reviews
“Very knowledgeable and friendly staff…”
Schedule Your Bone Grafting Consultation Today

Contact our Pittsburgh office directly to schedule your personalized consultation. At Pinnacle Center, our friendly and knowledgeable team is here to answer all your questions, discuss your treatment options, and ensure you feel comfortable and informed every step of the way. Trust Pinnacle Center to provide the highest quality periodontal care, enhancing your oral health, restoring functionality, and revitalizing your smile.